Health
Understanding Vaginal Prolapse: Causes, Symptoms, and Impact
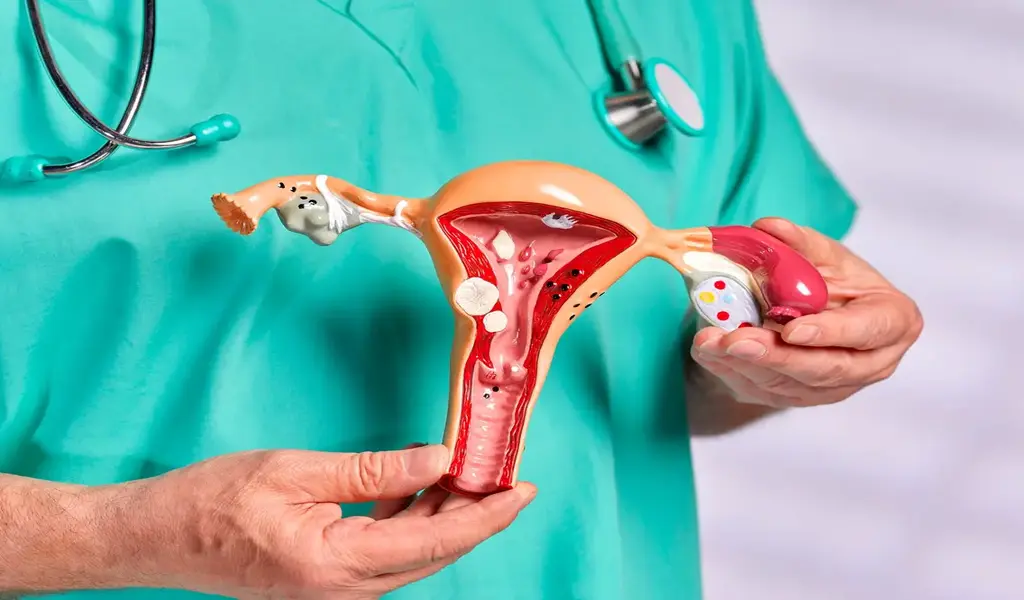
Vaginal prolapse is a condition that affects many women, especially as they age. To be more precise, experts estimate that about one-third of women may experience some degree of this affliction in their lifetime. It can have various causes, symptoms, and impacts on a woman’s life.
Understandably, vaginal prolapse sounds scary and concerning. But there is no need for fear. Instead, this article aims to provide a comprehensive overview of vaginal prolapse, helping you understand its causes, identify its symptoms, and impact. But most importantly, you will get crucial information on vaginal prolapse repair.
What is Vaginal Prolapse?
Vaginal prolapse is a medical condition where the pelvic organs, such as the bladder, uterus, or rectum, bulge or drop into the vaginal canal due to weakened or stretched pelvic muscles and ligaments. This phenomenon can result in discomfort, pain, and other complications if you fail to manage it or seek treatment.
Vaginal prolapse classification falls into various types based on the organ involved:
- Cystocele: Prolapse of the bladder into the vagina
- Urethrocele: Prolapse of the urethra into the vagina
- Uterine prolapse: Prolapse of the uterus into the vagina
- Rectocele: Prolapse of the rectum into the vagina
- Enterocele: Prolapse of the small intestines into the vagina
Causes of Vaginal Prolapse
Several factors can contribute to the development of vaginal prolapse. Some of the most common causes include:
- Pregnancy and childbirth
- Aging
- Menopause
- Chronic coughing
- Constipation
- Heavy lifting
- Obesity
Symptoms of Vaginal Prolapse
The symptoms of vaginal prolapse often vary and are contingent on the severity and type of prolapse. Some common signs and symptoms include:
- A sensation of heaviness or pressure in the pelvis
- A bulging feeling in the vagina
- Pelvic pain or discomfort
- Urinary and bowel problems
- Painful intercourse
- Back pain
Impact of Vaginal Prolapse on Women’s Lives
Vaginal prolapse can significantly impact your quality of life. It may affect your:
- Physical health: including chronic pain, discomfort, and complications from associated urinary or bowel problems.
- Sexual health: pain, discomfort, or embarrassment during sexual intercourse, which may negatively impact a woman’s sexual relationships and self-esteem.
- Mental health: feelings of anxiety, depression, and lowered self-esteem.
- Social life: Women with prolapse may avoid certain activities or social situations due to pain, discomfort, or embarrassment.
Vaginal Prolapse Treatment
Vaginal prolapse repair varies. However, there are various surgical procedures to correct the condition. The primary goal of these procedures is to relieve prolapse symptoms, restore pelvic anatomy, and improve your quality of life.
Types of Vaginal Prolapse Repair Procedures
The type of repair procedure depends on the specific form of prolapse, its severity, and your health condition. Some standard techniques include:
· Anterior repair (anterior colporrhaphy): This procedure targets the prolapse of the bladder (cystocele) or urethra (urethrocele) by tightening and strengthening the weakened vaginal wall.
· Posterior repair (posterior colporrhaphy): This surgery corrects the prolapsed rectum (rectocele) by repairing the damaged tissue between the vagina and rectum and reinforcing the vaginal wall.
· Vaginal hysterectomy: In cases of uterine prolapse, the doctor may remove the uterus (hysterectomy) through the vagina along with the repair of other prolapsed areas.
· Sacrocolpopexy: Doctors conduct this procedure for severe uterine or vaginal prolapse.
Please note that your medical provider may also recommend non-surgical approaches, such as pelvic floor exercises and lifestyle changes, for milder cases or as a complementary treatment to surgery. Conversely, they may prescribe inserting a vaginal pessary (for vaginal wall support) in moderate circumstances.
Conclusion
Understanding the causes, symptoms, and impact of vaginal prolapse can help you seek timely medical assistance, manage the condition effectively, and improve your quality of life. However, discussing all factors and potential risks with your healthcare provider before opting for any surgical intervention is essential.
SEE ALSO: Mosquitoes Strike Back: Local Malaria Resurfaces In The US After 20 Years