Health
Breast Cancer Screenings: Why Starting at Age 40 is Crucial for Early Detection
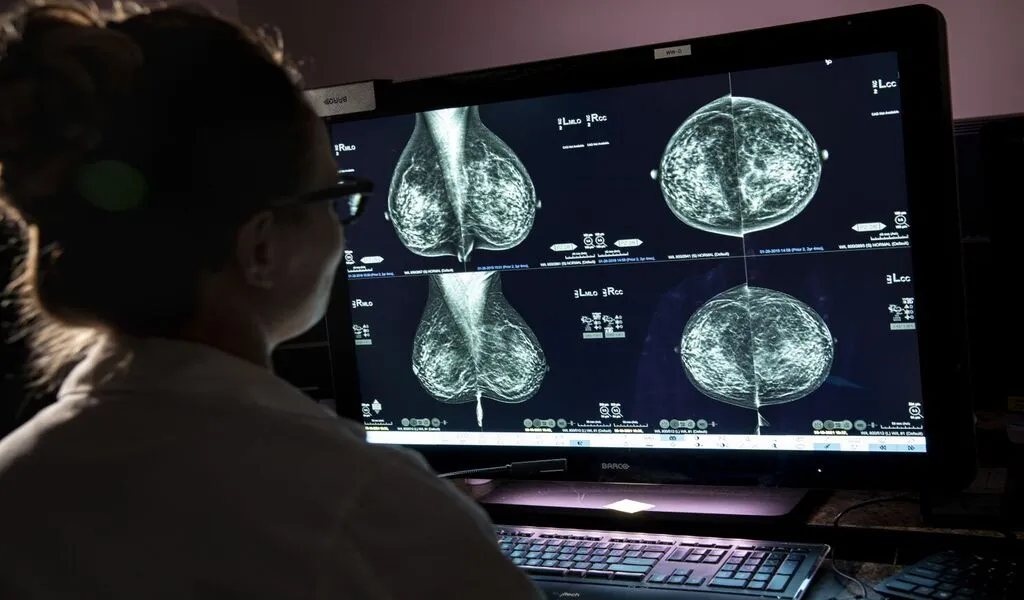
(CTN News) – Breast cancer is a significant health concern affecting millions of women worldwide. Early detection plays a crucial role in improving outcomes and saving lives.
However, there is an ongoing debate regarding the appropriate age to start breast cancer screenings. Current guidelines suggest initiating screenings at age 50, but evidence supports the argument that screenings should begin earlier, at age 40.
This article will explore the reasons behind this controversy and the potential benefits of starting breast cancer screenings at age 40.
Introduction
Breast cancer is the most common cancer among women globally, accounting for many cancer-related deaths. Detecting breast cancer at an early stage significantly increases the chances of successful treatment and long-term survival.
Mammography screenings have proven to be an effective tool in identifying breast cancer in its early stages. However, the age at which women should begin undergoing regular screenings is a topic of ongoing discussion and disagreement within the medical community.
Current guidelines for breast cancer screenings
The general consensus among major organizations, such as the American Cancer Society (ACS), is to recommend that women start regular breast cancer screenings at age 50.
These guidelines are based on extensive research and statistical analysis aimed at striking a balance between early detection and minimizing the potential harms associated with screenings.
However, this approach has drawn criticism from experts who argue that initiating screenings at age 50 may lead to missed opportunities for early detection.
The importance of early detection
Early detection of breast cancer is crucial for several reasons. Firstly, it allows for a greater range of treatment options, often resulting in less aggressive interventions and improved quality of life for patients.
Secondly, early-stage breast cancer is generally associated with higher survival rates than advanced-stage cancer. Lastly, early detection can significantly reduce healthcare costs by minimizing the need for extensive treatment and reducing the burden on the healthcare system.
The controversy surrounding the age for screenings
Arguments in favor of starting at age 40
Proponents of initiating breast cancer screenings at age 40 argue that this approach allows for detecting cancers that might otherwise go unnoticed. Breast cancer can occur at any age, and delaying screenings until age 50 may result in missed opportunities for early intervention.
Early detection offers the possibility of identifying smaller tumors, which are more likely to be treatable and have a better prognosis.
Arguments against starting at age 40
Opponents of starting screenings at age 40 raise concerns about the potential for false positives and unnecessary anxiety among women.
Mammograms may detect abnormalities that turn out to be benign, leading to additional tests, invasive procedures, and emotional distress.
Critics argue that the risks associated with false positives outweigh the benefits of early detection in younger women.
Benefits of starting screenings at age 40
Despite the controversy, several compelling arguments support the case for initiating breast cancer screenings at age 40.
Increased detection of early-stage breast cancer
Starting screenings at age 40 increases the likelihood of detecting early-stage breast cancer. Younger women have denser breast tissue, making it more challenging to identify abnormalities through physical examination alone.
Mammography screenings allow detecting tumors at an earlier stage, when they are smaller and more treatable. By starting screenings at age 40, healthcare providers can improve the chances of catching breast cancer in its early and more manageable stages.
Better survival rates
Early detection of breast cancer has a direct impact on survival rates. Studies have shown that women who undergo regular screenings starting at age 40 are more likely to survive breast cancer than those who start at age 50.
Detecting the disease early can initiate treatment promptly, leading to better outcomes and increased chances of long-term survival.
Reduced healthcare costs
While there are concerns about the potential costs associated with expanding breast cancer screenings to younger age groups, early detection can lead to long-term cost savings.
Treating breast cancer at advanced stages is often more expensive and requires more extensive interventions. By identifying and treating breast cancer earlier, healthcare systems can reduce the financial burden of advanced-stage cancer treatments.
Addressing the concerns against starting screenings at age 40
The concerns raised by opponents of starting screenings at age 40 are valid and should be taken into consideration. However, steps can be taken to mitigate these concerns.
Potential for false positives
False positives, where mammograms indicate the presence of cancer when none is present, can cause anxiety and lead to unnecessary follow-up procedures.
Improved screening techniques and protocols can be implemented to address this issue, such as digital mammography and supplementary tests like ultrasound or MRI when needed.
Refining screening methods can reduce the rate of false positives, providing a more accurate assessment of breast health.
Psychological impact on women
Screenings and the subsequent diagnostic process can be emotionally challenging for women. The fear and anxiety associated with the possibility of a cancer diagnosis should not be underestimated.
To address this concern, healthcare providers can enhance patient education and support, ensuring that women are well-informed about the benefits and limitations of screenings.
Open communication and compassionate care can help alleviate psychological distress and empower women to make informed decisions about their health.
The role of individual risk factors
It’s important to acknowledge that every woman’s risk of developing breast cancer is unique. While age is a significant risk factor, other factors such as family history, genetic predisposition, and personal health history should also be considered.
When to start breast cancer screenings should be based on an individual’s risk profile, considering a comprehensive health assessment and potential risk factors.
Personalized approaches to screening can optimize the balance between early detection and minimizing unnecessary interventions.
Empowering women to make informed decisions
The discussion surrounding the age to start breast cancer screenings should prioritize women’s empowerment in making informed decisions about their health.
Healthcare providers play a vital role in educating women about the benefits, risks, and limitations of screenings at different ages.
By fostering open and honest conversations, women can actively participate in their healthcare decisions, considering their values, preferences, and risk factors.
Importance of regular screenings
Regardless of the age at which screenings commence, the importance of regular breast cancer screenings cannot be overstated. Regular screenings enable healthcare providers to establish a baseline for breast health and detect any changes over time.
Following the recommended screening guidelines, whether it starts at age 40 or 50, increases the likelihood of detecting breast cancer at an early stage, leading to more effective treatment and improved outcomes.
The need for further research and personalized approach
The controversy surrounding the appropriate age for breast cancer screenings highlights the need for further research and a personalized approach to healthcare.
Ongoing studies can provide additional insights into the effectiveness and potential risks associated with screening at different ages.
Research efforts should focus on understanding the impact of early detection on survival rates, evaluating the benefits and harms of screenings in different age groups, and identifying effective strategies to minimize false positives and associated anxiety.
A personalized approach to breast cancer screenings is crucial. It should consider individual risk factors, preferences, and values.
Healthcare providers can collaborate with patients to develop tailored screening plans for their unique circumstances. This approach ensures that screenings are not solely based on age but consider a comprehensive assessment of each woman’s risk profile.
Incorporating advanced technologies and innovative screening methods can also improve breast cancer screenings’ accuracy and effectiveness. Ongoing advancements in imaging techniques, such as 3D mammography and molecular breast imaging, promise to enhance early detection capabilities.
In conclusion, the age at which breast cancer screenings should start is a complex and debated topic. While current guidelines recommend initiating screenings at age 50, there is a strong argument for starting at age 40.
Early detection of breast cancer can lead to improved outcomes, higher survival rates, and reduced healthcare costs. Addressing false positives and psychological impact concerns is crucial, and a personalized approach that considers individual risk factors is essential.
Regardless of starting age, regular screenings remain vital in detecting breast cancer early. Further research and advancements in technology will continue to shape the guidelines and provide women with the best possible care.
Related CTN News: