Health
India’s Fight Against Malaria: Point-Of-Care Diagnostics And Technologies
(CTN News) – India lacks the capacity to cope with disease burden Malaria despite a significant pool of brilliant healthcare professionals.
Malaria is a preventable disease that kills many lives every year in rural and remote areas and even Tier-3 and 4 towns without healthcare coverage.
The Southeast Asian region has done well and malaria cases have fallen by 76% in the new millennium, but still accounts for about 2% (5.4 million cases in 2021) of global cases. It is estimated that 79% of these cases and more than 82% of malaria-related deaths occur in India.
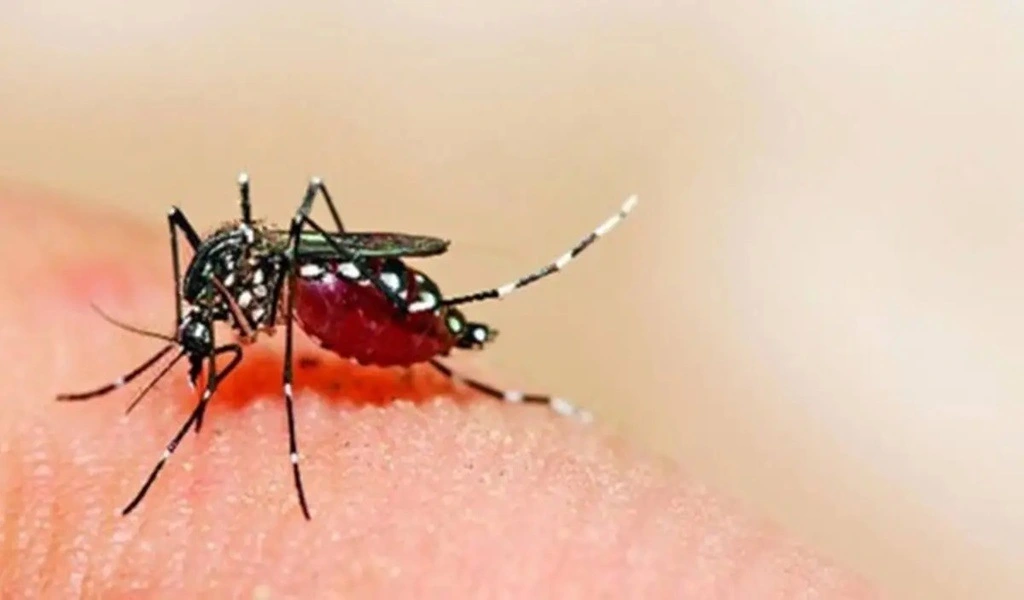
Since malaria is a parasitic infection transmitted to humans through the bite of infected mosquitoes, prompt diagnosis is essential for timely and successful treatment.
Conventional methods of malaria diagnosis in India
The malaria parasite is detected by microscopy, which involves examining a sample of blood under a microscope to determine whether it contains malaria parasites.
It is one of the most conventional and accurate testing methodologies, but it requires qualified healthcare professionals and sophisticated equipment. Furthermore, it may take several hours for the results to be available.
This is a molecular technique used to identify the genetic material of a parasite in a patient’s blood sample using Polymerase Chain Reaction (PCR).
Although it is a highly sensitive and specific way of analyzing samples, it suffers from the same limitations as microscopy, including the need to purchase specialized equipment, train medical professionals, and take a long time to produce a final report.
Rural areas in India lack such specialized facilities and equipment, which is a major reason for the low rate of timely detection of malaria infections.
Fortunately, now that point-of-care diagnostic devices and technologies have been introduced, all the above-mentioned shortcomings that rural India faces can be addressed.
The effectiveness of POC diagnostic devices can be attributed to several factors.
A POC device is a portable diagnostic tool that is easy to use. While these devices offer medical grade accuracy of diagnosis and may be used at the point of care itself, they do not require a professional medical background to operate them.
As a result, they can be seamlessly integrated into rural areas with very limited resources.
There are now a variety of POC devices being used in diverse settings, such as primary health centers and community health centers, and even by rural entrepreneurs who acquire and learn how to use them for door-to-door testing and diagnosis of infections such as malaria.
It is through such deployments that POC devices become more convenient, cost-effective, and easily accessible for patients.
Further, unlike laboratory-based testing, where patients are tested and receive results hours or even days later, POC diagnostic devices usually provide results within seconds or 10-15 minutes.
Furthermore, these devices are often battery-operated and are capable of sending test results and patient information electronically to doctors located in hospitals. It is possible to provide telemedicine and video consultations to patients without delay, and malaria infections can be prevented from progressing if detected early enough.
Through rapid diagnostic tests (RDTs), POC devices enable the identification of malaria parasites.
SEE ALSO:
A New AHIP Ad Takes On Big Pharma’s Prices




























