Health
HPV Vaccine Uptake Among High-Income Groups Is Low
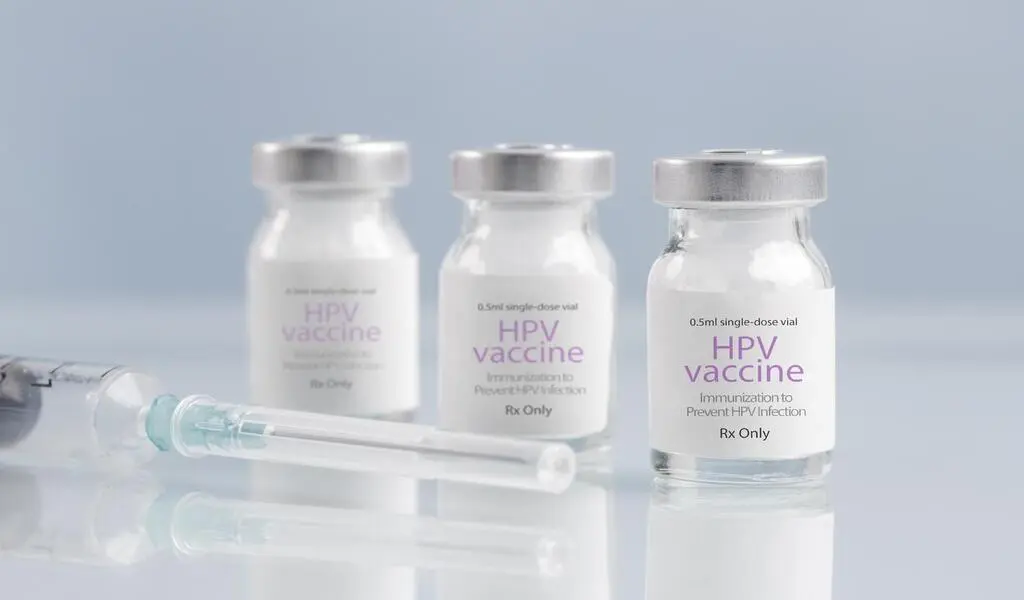
(CTN News) – Vaccination rates for children against human papillomavirus (HPV) are lower among parents with higher socioeconomic status, and reasons for hesitancy differ among income groups, a study finds.
Herd immunity may be undermined by perceptions about vaccines in higher-income groups. The Lancet Regional Health published the findings of a team at Medical University of South Carolina (MUSC).
US health officials aim to fully vaccinate 80% of adolescents by 2030, but uptake of the HPV vaccine lags at 63% for teens, as HPV can cause six kinds of cancer. Women born between 1988 and 1996 who were fully vaccinated as adolescents in a recent study from Scotland found dramatic results. In the group, no cervical cancer cases were found.
Disparities have already been reversed
They wanted to sift out the reasons behind the higher HPV coverage rates in low-income and minority communities. A telephone survey that covers routine immunizations, the National Immunization Survey-Teen, was used to examine possible reasons.
A study found that 65% of parents from socioeconomically advantaged backgrounds did not intend to vaccinate their teenage children, compared with 40% of parents from disadvantaged backgrounds. Across both groups, the study indicates a pervasive lack of intent to vaccinate against HPV.
HPV Various reasons were given for hesitancy
Researchers found that advantaged parents were concerned about vaccine safety. Parents from disadvantaged groups, on the other hand, said they were unaware of the HPV vaccine, did not have a health provider’s recommendation, or did not think the vaccine was necessary.
Kalyani Sonawane, PhD, the lead study author, said parents from advantaged groups may overestimate the HPV vaccine’s side effects. The low uptake in that group raises concerns about broader issues.
Considering most adolescents are white, from middle- and high-income families, and their parents are skeptical about vaccine safety, this affects the coverage of vaccines at the population level, she explained.
Risks are significant for both income groups, according to researchers. Recent studies indicate rising cervical cancer rates among White women in low-income countries and among women in their 30s, particularly among Black and Hispanic women.
Young adults’ uptake gap related to pandemics
This week, Sonawane and some of the Lancet study’s authors published new findings about HPV vaccination during the COVID pandemic. A research letter in JAMA Network Open detailed their findings.
A study focused on participants ages 18 to 26 years old in 2018, 2019, and 2022 was conducted using data from the National Health Interview Study. More than half of the participants were women.
Young adults’ HPV coverage did not increase during the pandemic, compared to the prepandemic period, likely due to pandemic-related disruptions. Males and females without health insurance had lower coverage rates.
Comparing lesbians, gay men, bisexuals, and other sexual orientation groups with heterosexuals, the investigators found higher rates.
In those groups, the researchers said, the higher rates were reassuring because their risk was higher. Uninsured people, however, were less likely to get the HPV vaccine, which underscores the need for easier access to the vaccine.
SEE ALSO:
What Role Chiropractic Care Plays in Managing Chronic Pain: Insights and Evidence