Health
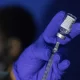
Thailand’s Ministry of Public Health Tells Hospitals to Prescribe Antibiotics Less Often
CHIANG RAI – The Ministry of Public Health has instructed all hospitals under it’s authority to prescribe medications appropriately, and lower antibiotics use by 20%, by 2021.
In 2019, the ministry will decrease antibiotic prescriptions for upper respiratory tract infections, acute diarrhea, open wounds and normal labor, to decrease drug resistant risks. The ministry instructed the hospitals to prescribe medications appropriately to patients suffering from non-communicable diseases such as hypertension and diabetes, as well as high-risk patients such as senior people, pregnant women, chronic kidney patients and patients who require consistent and continuous medicine.
The ministry also instructed 125 large hospitals nationwide to develop an integrated antibiotic resistance management system, with the goal to decrease antibiotic prescription by 20% and antimicrobial resistance illnesses by 50%.
An average of two people die every hour from multidrug-resistant bacterial infections in Thailand, according to a landmark study funded by the kingdom’s health ministry and Britain’s Wellcome Trust, and published in September of 2018.
The study used micromicrobiology databases, hospital admission databases and the national death registry to estimate that multidrug-resistant bacterial infections killed 19,122 people in Thailand in 2010. Thailand’s population is 68 million.
IT’S IN YOUR MEAT TOO
Antibiotics used on livestock is another concern. Drug-resistant bacteria spreads through direct contact between humans and farm animals, ingested meat or the environment.
In many large industrial farms, where cramped conditions allow diseases to spread fast, antibiotics are often used on healthy animals to prevent rather than treat illnesses.
According to Thailand’s National Antimicrobial Resistance Surveillance Centre website, the kingdom uses about 10 billion baht worth of antibiotics every year. It is unclear how much is used on animals.
Thailand’s Food and Drug Administration as well as the Department of Livestock Development did not respond to requests for interviews.
While farmers in Thailand are banned from using antibiotics as growth promoters, experts say there are still information gaps on how and where the drugs are used on farms. This is something the Food and Agriculture Organisation (FAO) is working with the Thai government to fix, along with raising awareness of the problem.
Dr Wantanee Kalpravidh, an FAO regional manager, thinks the stringent standards set by countries importing Thailand’s farmed products motivate companies to rein in antibiotic use. But cutting back on its use may not save money, since farms need to vaccinate the animals and put up biosafety barriers to protect the animals from disease.
She suggests governments consider dangling incentives before conscientious farmers. “Can the government recognise this as corporate social responsibility and reduce their tax?” she said.
After all, the benefits from reducing indiscriminate use of antibiotics extend to the larger society, and go beyond borders.
It will help lower healthcare costs, for one thing. At Bangkok’s public Ramathibodi Hospital, staff have to wear a 12-baht, one-time-use protection gown every time they approach a patient infected with a superbug. Staff in one intensive care ward with 20 of these patients go through 10,000 such gowns a month, reveals the hospital’s deputy director Kumthorn Malathum.
In conjunction with World Antibiotics Awareness Week starting on Nov 14, the hospital will set up information booths to educate patients about proper use of antibiotics. “People don’t often see the long-term effects caused by superbugs,” says Dr Kumthorn. “People think patients just die quickly and the (treatment) cost is low. But infection caused by superbugs also affects your long-term quality of life.”
Mr Songchai’s troubles began earlier this year, when he fell while going down the stairs at home.
His knees hurt so much he resorted to taking an over-the-counter muscle relaxant three times a day, on top of a cocktail of four to five drugs for diabetes, high blood pressure and other ailments.
The combination of drugs proved too much for his kidneys, so he had to undergo temporary dialysis. It was during the treatment that he was felled by the drug-resistant superbug.
The avid golf and billiards player is now reduced to watching such tournaments on television at home.
He scribbles glumly on a piece of paper: “Don’t use (antibiotics) by yourself. Ask the doctor first.”