Health
Mpox Outbreak In Congo Raises Concerns Of Discrimination Against LGBTQ+ Communities
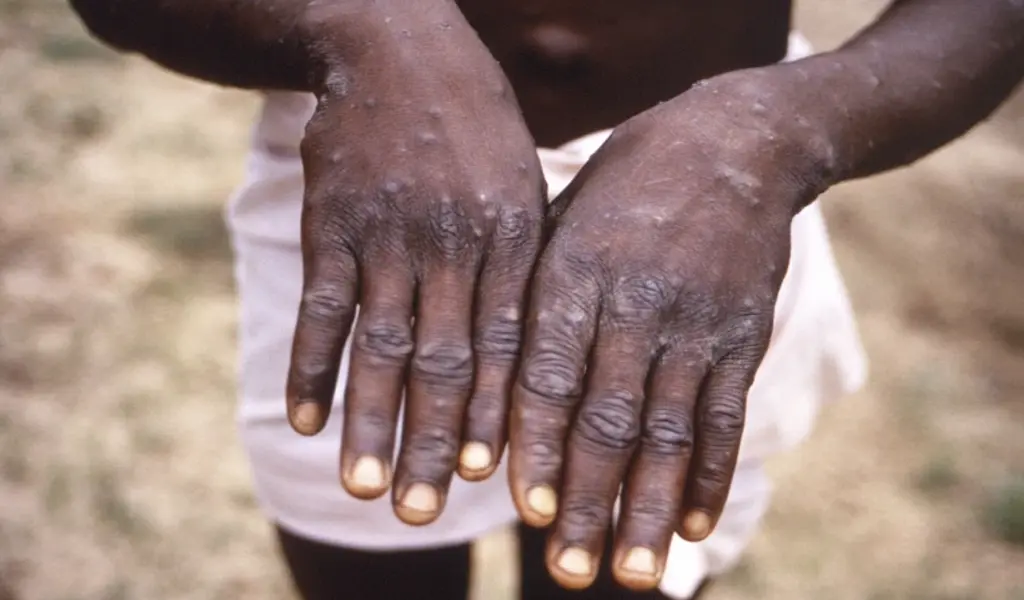
(CTN News) – As the Democratic Republic of the Congo grapples with its most significant outbreak of monkeypox, scientists are sounding the alarm about the potential exacerbation of the situation due to discrimination against gay and bisexual men on the continent.
In a November report, the World Health Organization revealed a noteworthy development in the transmission of monkeypox, also known as mpox, indicating its spread through sexual contact in Congo for the first time.
This represents a marked departure from previous occurrences, where the virus primarily affected individuals in close proximity to infected animals.
While monkeypox has been present in various parts of central and west Africa for decades, it wasn’t until 2022 that its transmission through sexual means was officially documented.
Strikingly, the majority of the approximately 91,000 people infected across approximately 100 countries that year were identified as gay or bisexual men.
In the African context, the reluctance to report symptoms could potentially drive the outbreak underground, warns Dimie Ogoina, an infectious diseases specialist at Niger Delta University in Nigeria.
This underreporting poses a significant challenge to effective containment and mitigation efforts, further emphasizing the need for inclusive and non-discriminatory public health strategies in addressing the monkeypox outbreak.
Dimie Ogoina, an infectious diseases specialist at Niger Delta University in Nigeria, highlighted a potential link between the prohibition of homosexuality by law in most parts of Africa and the hesitancy of individuals to come forward if they suspect they have been infected with mpox.
The World Health Organization (WHO) officials reported the identification of the first sexually transmitted cases of the more severe type of mpox in Congo last spring.
This discovery followed the arrival of a Belgian resident in Kinshasa, the Congolese capital, who identified as a man engaging in sexual relations with other men. Subsequently, five other individuals who had sexual contact with the man also contracted mpox.
Ogoina, along with his colleagues, had previously reported in 2019 that mpox might be spreading through sexual transmission. However, gaps in monitoring make it challenging to accurately estimate the number of mpox cases linked to sexual transmission.
Despite this, a significant number of mpox cases in Nigeria involve individuals with no known contact with animals.
Challenges in Addressing Mpox Outbreak in Congo: Limited Confirmations, Sexual Transmission, and Stigma
In Congo, where about 13,350 suspected cases of mpox have been reported, including 607 deaths as of the end of November, only around 10% of cases have been confirmed by laboratories.
The extent to which infections were spread through sexual contact remains unclear, but WHO noted that approximately 70% of cases are in children under 15.
During a recent assessment trip to Congo, WHO officials found a lack of awareness among health workers regarding the sexual transmission of mpox, leading to missed cases.
The health agency confirmed sexual transmission of mpox between male partners and simultaneously through heterosexual transmission in different parts of the country.
Mpox typically manifests symptoms such as fever, skin rash, lesions, and muscle soreness for up to one month. It is primarily spread through close contact, and most individuals recover without requiring medical treatment.
While mass vaccination programs were implemented in some countries during the 2022 international outbreak, experts suggest that replicating such programs in Africa may face challenges, including the stigma against gay communities.
Dr. Boghuma Titanji, an assistant professor of medicine in infectious diseases at Emory University School of Medicine in Atlanta, expressed skepticism about the likelihood of a similar demand for vaccines in Africa as seen in the West.
She emphasized the importance of finding ways to administer shots, if available, without stigmatizing the gay and bisexual communities most at risk of mpox.
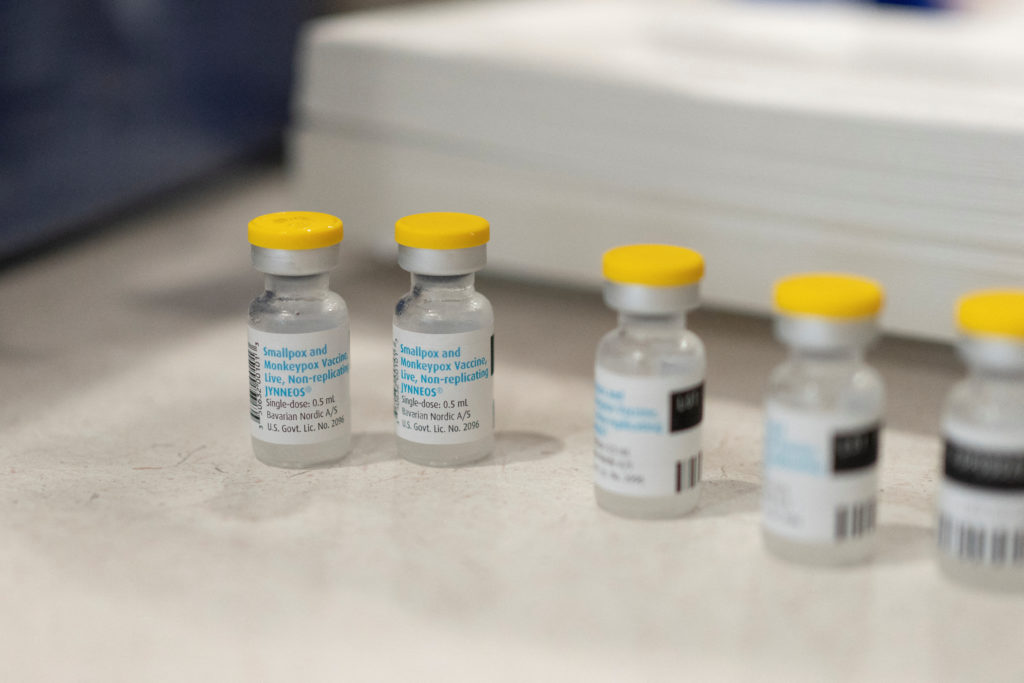
FILE PHOTO: Vials of the JYNNEOS smallpox and monkeypox vaccine are placed on a table during a clinic offered by the Pima County Department of Public Health at Abrams Public Health Center in Tucson, Arizona, U.S., August 20, 2022. REUTERS/Rebecca Noble/File Photo
Dr. Jean-Jacques Muyemba, the general director of Congo’s National Institute of Biomedical Research, expressed concern about the emergence of clusters of mpox spread through sexual contact in two provinces of Congo.
This development is particularly troubling given the lack of a licensed vaccine in Congo, and obtaining a sufficient number of shots for a large-scale program is proving challenging.
The country is striving to acquire a Japanese mpox vaccine, but regulatory obstacles are complicating the situation.
On a global scale, only one vaccine against mpox has been authorized, produced by Denmark’s Bavarian Nordic.
However, the supply is extremely limited, and even if available, approval by the African countries or the World Health Organization (WHO) would be necessary for their use. So far, the vaccine has been accessible in Congo exclusively through research initiatives.
Key Insights from Experts on Mpox Outbreak in Africa
Oyewale Tomori, a Nigerian virus expert affiliated with several WHO advisory boards, suggested that African governments might hesitate to seek assistance from the U.N. health agency or donors for vaccine procurement due to numerous competing priorities.
He emphasized that, in Africa, mpox is likely considered a low-priority concern.
Instead, he advocated for strengthening monitoring systems, expanding laboratory networks, and ensuring better availability of diagnostic supplies as more practical measures for the continent than vaccines.
Dimie Ogoina warned that without increased efforts to halt the outbreaks in Africa, mpox is likely to continue infecting new populations.
He cautioned that the disease could potentially lead to outbreaks in other countries, reminiscent of the global emergency declared by WHO last year.
Ogoina drew parallels with the initial stages of the HIV pandemic, which started among gay and bisexual men in the global north. At the time, Africa perceived it as a distant problem, but eventually, the virus spread to the continent, affecting heterosexual populations.
Currently, women of reproductive age account for over 60% of new HIV infections in Africa, raising concerns that a similar scenario might unfold with mpox unless proactive measures are taken to address the outbreaks in the region.
Ogoina emphasized the importance of addressing these challenges to prevent the recurrent resurgence of the virus.