(CTN NEWS) – In 2016, hospitals in New York made a startling discovery – a rare and serious fungal illness, Candida auris, which had never been reported in the United States before.
Further investigations by research laboratories revealed that the fungus had been present in the country since at least 2013, prompting concerns about its prevalence.
Since its initial detection, New York City has become the epicenter of Candida auris infections.
While the virus has spread to other locations, New York state consistently recorded the highest number of confirmed cases in the nation every year until 2021, as per data from the Centres for Disease Control and Prevention (CDC), analyzed by The Associated Press.
Candida auris poses an increasingly serious public health risk, as it can lead to severe illnesses like bloodstream, wound, and respiratory infections.
Its estimated death rate of 30% to 60% makes it a significant concern, especially for patients with major medical conditions in healthcare facilities.
Last year, patients in 29 states had the fungus clinically recognized, with Nevada and California reporting the highest number of instances. However, New York remains a key hotspot for the infection.
Traditionally, most fungal pathogens struggled to survive in mammal bodies, including humans, due to body temperatures. This provided some protection against infections.
However, as temperatures rise, fungi may adapt to warmer settings, potentially reducing human resistance. Studies suggest that Candida auris is already undergoing such adaptation.
Interestingly, Candida auris appeared on three continents simultaneously 14 years ago, in Venezuela, India, and South Africa, surprising experts due to the diverse climates in these regions.
Arturo Casadevall, a microbiologist, immunologist, and professor at Johns Hopkins University specializing in fungus diseases, pointed out the significance of this occurrence.
As Candida auris continues to pose challenges to public health, researchers and healthcare authorities are closely monitoring its spread and working towards effective prevention and treatment strategies.
The Warming Planet: Candida Auris’ Challenge to Mammals’ Warmth Defense
With warmth providing mammals an excellent defense against environmental fungi, there is concern that certain fungi will breach the temperature barrier if the planet continues to warm.
According to Casadevall, some fungi now possess higher temperature tolerances, a departure from history when warm body temperatures safeguarded mammals.
Initially linked to patients who had traveled to the United States from other countries, instances of Candida auris are now predominantly acquired locally, spreading among patients in medical settings, as stated by Meghan Marie Lyman, a CDC medical epidemiologist for the mycotic diseases branch.
The United States witnessed a dramatic surge in confirmed clinical cases, with 2,377 detected last year, marking an increase of over 1,200% from 2017. Notably, Candida auris is spreading globally, with case counts in Europe nearly doubling between 2020 and 2021, according to a survey.
Despite improved screens and surveillance, the geographic spread of the infection has expanded along with the rising number of cases, as observed by Lyman.
The CDC highlighted the pathogen’s resistance to conventional antifungal treatments and its alarming rate of spread in a news release in March, emphasizing the urgency of transmission mitigation techniques in healthcare settings.
Dr. Luis Ostrosky, an infectious diseases professor at McGovern Medical School at UTHealth Houston, described Candida auris as a “nightmare scenario.”
It possesses the potential for multi-drug resistance and rapid dissemination in medical facilities, distinguishing it as a unique challenge in the realm of fungal infections.
Challenging Candida Auris: A Resistant and Elusive Fungal Threat
Candida auris, a formidable fungal infection, often exhibits resistance to the most widely used class of antifungal drugs, and occasionally even to another drug prescribed for serious catheter fungal infections in hospitals.
Dr. Ostrosky, who has treated about ten patients with this fungus and advised many others, shared his disheartening experiences of having to inform families that no effective treatment is available for their loved ones suffering from the infection.
He witnessed its rapid spread throughout an entire Intensive Care Unit in just two weeks.
Researchers, academics, and public health organizations are actively exploring theories to explain the emergence of Candida auris. Among the most widely recognized theories is climate change, according to Dr. Ostrosky.
It is believed that the fungus might have always existed among the bacteria inhabiting the human body, but its potential health risks were overlooked until it began causing infections.
While reports of the fungus in natural environments like soil and wetlands exist, environmental sampling has been limited, and its origins and potential human involvement remain uncertain.
The complex interplay of human interaction with nature, environmental changes, and the use of fungi in agriculture might have allowed Candida auris to adapt and spread into new environments, leaving many unanswered questions.
Regardless of its origins, the fungus poses a significant threat to human health.
Immunocompromised individuals in hospitals are particularly vulnerable, but long-term care facilities and nursing homes also face risks due to limited access to diagnostics and infection control specialists.
Diagnosing Candida auris is challenging, as it mimics common signs of infection like sepsis, fever, and low blood pressure, which can have various causes. The rarity of the infection means that many doctors might not even be aware of its existence.
Treatment is equally problematic, with limited options available. The difficulty in diagnosis and treatment underscores the urgency of understanding and combating this elusive and dangerous fungal pathogen.
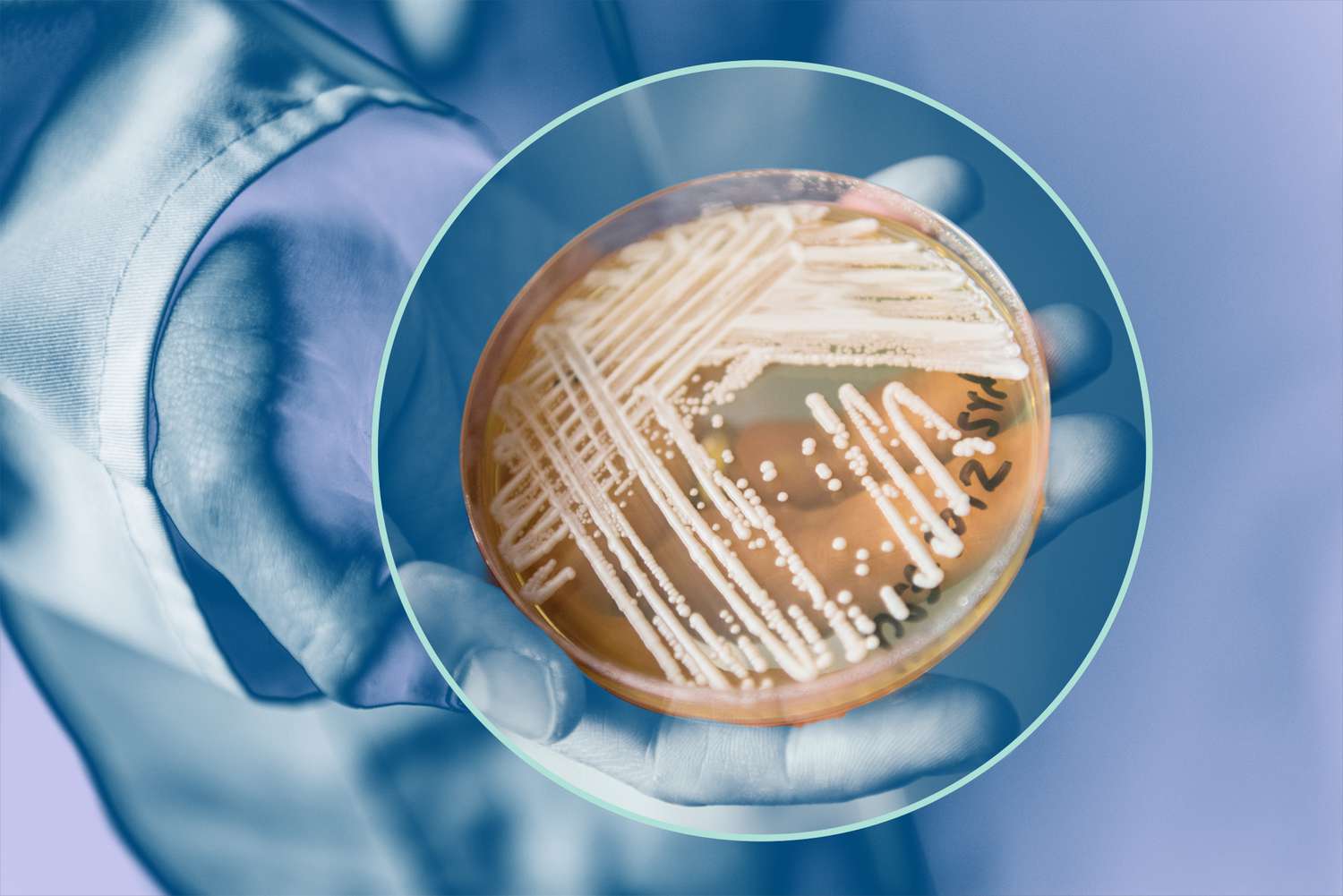
Blood tests are used to identify the fungus, but even detecting its presence can be a complex process, involving specialized nutrient-rich mediums to encourage growth and facilitate detection of infectious organisms.
Detection Challenges and Humorous “Gold Standard” for Candida Auris Cases
Ostrosky points out, however, that relying solely on current detection methods misses approximately 50% of the Candida auris cases. While more recent equipment is available to enhance bloodstream detection, its high cost and limited usage in hospitals remain barriers.
He humorously remarks that their current “gold standard” for detection is only slightly better than flipping a coin.
In addition to the rise in incidence, popular culture has played a role in increasing public awareness of fungal infections.
The HBO drama “The Last of Us” revolves around surviving a fungus outbreak, blurring the line between science fiction and the real challenge of combating climate change, which is reshaping the landscape of diseases posing major threats to human health.
Johns Hopkins researcher Casadevall explains that global warming exerts selection pressure on microbes through the increasing frequency of extremely hot days.
Each day with temperatures above 100 degrees Fahrenheit (37.7 degrees Celsius) becomes a selection event for microbes, and the more such days occur, the higher the probability that some will adapt and survive.
Ostrosky reflects on how mycology has been relatively overlooked for decades, as fungal infections were not as commonly seen before.
However, with the emergence of challenging pathogens like Candida auris, the spotlight is now on fungal diseases and the urgent need to understand, detect, and treat them effectively.
RELATED CTN NEWS:
Thailand Parliament’s Joint Meeting: Postpones Parliamentary PM Vote Scheduled For Aug 4th