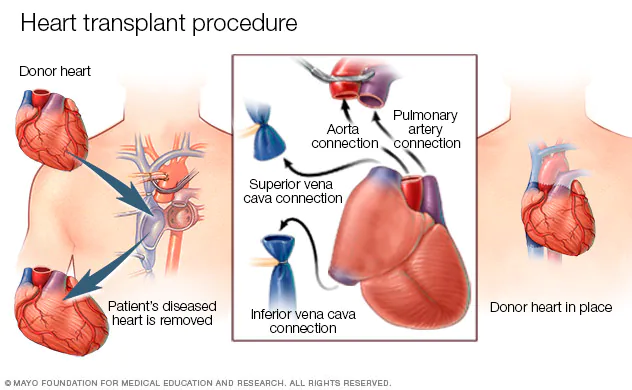
(CTN NEWS) – Heart transplantation is a complex surgical procedure that involves replacing a damaged or diseased heart with a healthy donor heart.
It is considered a life-saving treatment option for individuals with end-stage heart failure or certain heart conditions that cannot be managed through other interventions.
This article explores the process of heart transplantation, the criteria for eligibility, the surgery itself, and the recovery process.
Understanding Heart Failure
Heart failure is a serious condition in which the heart becomes weak and unable to pump blood efficiently throughout the body.
This can be caused by various factors such as coronary artery disease, heart valve problems, or cardiomyopathy.
When all other treatment options have been exhausted and the patient’s quality of life is significantly compromised, heart transplantation may be considered.
Eligibility for Heart Transplantation
Heart transplantation is a major surgical procedure, and not all individuals with heart failure are eligible candidates.
The selection process involves careful evaluation by a multidisciplinary team of healthcare professionals, including cardiologists, surgeons, and psychologists.
The following criteria are typically considered when assessing eligibility for heart transplantation:
- Severe Heart Failure: The patient should have end-stage heart failure with symptoms that significantly impact their quality of life, such as severe fatigue, shortness of breath, and fluid retention.
- Age and Overall Health: While age alone is not a determining factor, younger patients tend to have better outcomes. The patient should also have an overall good health status, with no significant organ dysfunction or other conditions that may affect the success of the transplant.
- Absence of Contraindications: Certain medical conditions, such as active infections, cancer, or irreversible liver or kidney disease, may pose a risk during or after the transplantation process. These conditions are thoroughly evaluated to determine if they are manageable or disqualifying.
- Psychosocial Assessment: A comprehensive assessment of the patient’s psychological and social well-being is conducted to ensure they have the necessary support systems in place to cope with the demands of the transplant process and post-transplant care.
The Transplantation Process
Once a patient has been deemed eligible for heart transplantation, they are placed on the waiting list for a suitable donor heart.
The waiting period can vary widely and largely depends on factors such as blood type compatibility, body size, and severity of illness.
During this time, patients are closely monitored and supported to manage their symptoms and maintain their overall health.
When a suitable donor heart becomes available, a transplant surgical team is assembled, and the patient is promptly notified. The surgical procedure involves several steps:
- Anesthesia: The patient is put under general anesthesia to ensure they are unconscious and pain-free throughout the procedure.
- Incision: A large incision is made in the chest to access the heart. This is typically done through a sternotomy, where the breastbone is divided, allowing the surgeon access to the heart.
- Removal of the Diseased Heart: The surgeon carefully disconnects the patient’s heart from the surrounding blood vessels and removes it from the chest.
- Implantation of the Donor Heart: The healthy donor heart is then transplanted into the recipient’s chest. The surgeon connects the blood vessels and carefully sutures them to ensure proper blood flow.
- Connection of the Heart to Life-Support Systems: Once the new heart is in place, the surgical team connects the patient to a heart-lung machine, which temporarily takes over the pumping function until the new heart begins to function effectively.
- Closure: The incision is closed using surgical sutures or staples, and the chest is carefully bandaged.
Post-Transplant Recovery
Following heart transplantation, the patient is closely monitored in the intensive care unit (ICU) to ensure the stability of the new heart and manage any potential complications.
The length of the ICU stay varies depending on the individual’s progress and any post-operative issues that may arise.
Once the patient is stable, they are transferred to a regular hospital room for further recovery.
During this time, they undergo rehabilitation, which includes physical therapy, medication management, and education on post-transplant care.
Long-term success and well-being following heart transplantation require strict adherence to a lifelong regimen of medications to prevent organ rejection.
Regular follow-up appointments with the transplant team are essential to monitor the patient’s progress, adjust medications as needed, and address any concerns or complications that may arise.
Conclusion
Heart transplantation is a life-saving procedure that offers hope and improved quality of life to individuals with end-stage heart failure.
Through careful evaluation, surgical expertise, and comprehensive post-transplant care, this procedure has transformed the lives of countless individuals worldwide.
While it is not without risks and challenges, heart transplantation remains a remarkable medical achievement that continues to push the boundaries of what is possible in the field of cardiac care.
RELATED CTN NEWS:
Condom Size Chart: Finding The Perfect Fit For Maximum Comfort And Protection
5 Surprising Facts About Human Metapneumovirus That Will Leave You Breathless!
Stiff Person Syndrome Symptoms: Understanding The Signs And Treatment Options