Health
Fighting Cervical Cancer With Vinegar and Ingenuity
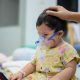
Anuree Talasart, a nurse provider in Roi Et Province, Thailand, teaches a group of women about the female reproductive system.
Maikaew Panomyai did a little dance coming out of the examination room, switching her hips, waving her fists in the air and crowing, in her limited English: “Everything’s O.K.! Everything’s O.K.!”
Translation: The nurse just told me I do not have cervical cancer, and even the little white spot I had treated three years ago is still gone.
What allowed the nurse to render that reassuring diagnosis was a remarkably simple, brief and inexpensive procedure, one with the potential to do for poor countries what the Pap smear did for rich ones: end cervical cancer’s reign as the No. 1 cancer killer of women. The magic ingredient? Household vinegar.
Every year, more than 250,000 women die of cervical cancer, nearly 85 percent of them in poor and middle-income countries. Decades ago, it killed more American women than any other cancer; now it lags far behind cancers of the lung, breast, colon and skin.
Nurses using the new procedure, developed by experts at the Johns Hopkins medical school in the 1990s and endorsed last year by the World Health Organization, brush vinegar on a woman’s cervix. It makes precancerous spots turn white. They can then be immediately frozen off with a metal probe cooled by a tank of carbon dioxide, available from any Coca-Cola bottling plant.
The procedure is one of a wide array of inexpensive but effective medical advances being tested in developing countries. New cheap diagnostic and surgical techniques, insecticides, drug regimens and prostheses are already beginning to save lives.
With a Pap smear, a doctor takes a scraping from the cervix, which is then sent to a laboratory to be scanned by a pathologist. Many poor countries lack high-quality labs, and the results can take weeks to arrive.
Women who return to distant areas where they live or work are often hard to reach, a problem if it turns out they have precancerous lesions.
Miss Maikaew, 37, could have been one of them. She is a restaurant cashier on faraway Ko Chang, a resort island. She was home in Poyai, a rice-farming village, for a brief visit and was screened at her mother’s urging.
The same thing had happened three years ago, and she did have a white spot then. (They resemble warts, and are caused by the human papillomavirus.) It was frozen off with cryotherapy, which had hurt a little, but was bearable, she said.
Thailand is a leader in adopting the cryotherapy technique.
Since she has been screened twice in her 30s, her risk of developing cervical cancer has dropped by 65 percent, according to studies by the Alliance for Cervical Cancer Prevention, a coalition of international health organizations funded by the Bill & Melinda Gates Foundation.
The procedure, known as VIA/cryo for visualization of the cervix with acetic acid (vinegar) and treatment with cryotherapy, can be done by a nurse, and only one visit is needed to detect and kill an incipient cancer.
Thailand has gone further than any other nation in adopting it. More than 20 countries, including Ghana and Zimbabwe, have done pilot projects. But in Thailand, VIA/cryo is now routine in 29 of 75 provinces, and 500,000 of the 8 million women, ages 30 to 44, in the target population have been screened at least once.
Dr. Bandit Chumworathayi, a gynecologist at Khon Kaen University who helped run the first Thai study of VIA/cryo, explains that vinegar highlights the tumors because they have more DNA, and thus more protein and less water, than other tissue.
It reveals pre-tumors with more accuracy than a typical Pap smear. But it also has more false positives — spots that turn pale but are not malignant. As a result, some women get unnecessary cryotherapy.
But freezing is about 90 percent effective, and the main side effect is a burning sensation that fades in a day or two.
By contrast, biopsies, the old method, can cause bleeding.
“Some doctors resist” the cryotherapy approach, said Dr. Wachara Eamratsameekool, a gynecologist at rural Roi Et Hospital who helped pioneer the procedure. “They call it ‘poor care for poor people.’ This is a misunderstanding. It’s the most effective use of our resources.”
At a workshop, nurse trainees pored over flash cards showing cervixes with diagnosable problems. They did gynecological exams on lifelike mannequins with plastic cervixes. They performed cryotherapy on sliced frankfurters pinned deep inside plastic pipes. Then, after lunch, they broke into small groups and went by minibus to nearby rural clinics to practice on real women.
Because cervical cancer takes decades to develop, it is too early to prove that Thailand has lowered its cancer rate. In fact, Roi Et Province, where mass screening first began, has a rate higher than normal, but doctors attribute that to the extra testing. But of the 6,000 women recruited 11 years ago for the first trial, not a single one has developed full-blown cancer.
VIA/cryo was pioneered in the 1990s simultaneously by Dr. Paul D. Blumenthal, an American gynecologist working in Africa, and Dr. Rengaswamy Sankaranarayanan in India.
Dr. Blumenthal said he and colleagues at the Johns Hopkins medical school had debated ways to make cervical lesions easier to see, and concluded that whitening them with acetic acid would be effective. Freezing off lesions is routine in gynecology and dermatology; the challenge was making it cheap and easy. Liquid nitrogen is hard to get, but carbon dioxide is readily available.
Thailand seems made for the vinegar technique. It has more than 100,000 nurses and a network of rural clinics largely run by them.
Also, while poor rural villagers in many countries go to shamans or herbalists before they see doctors, poor Thais do not. Thailand has a 95 percent literacy rate, and doctors are trusted. The king is the son of a doctor and a nurse; his father trained at Harvard. One of the royal princesses has a doctorate in chemistry and an interest in cancer research.
But the real secret, Dr. Wachara said, is this: “Thailand has Lady Kobchitt.”
Dr. Kobchitt Limpaphayon to her colleagues at Bangkok’s Chulalongkorn University medical school and “Kobbie” to her classmates long ago at New York’s Albany Medical College, she is the gynecologist to the Thai royal family. “Kobbie is a force of nature,” said Dr. Blumenthal, who has taught with her. In 1971, as a young doctor, she moved from Albany to Baltimore to help start the Johns Hopkins Program for International Education in Gynecology and Obstetrics.
In 1999, she read one of Dr. Blumenthal’s papers and asked him to introduce VIA/cryo in Thailand. Without her connections and powers of persuasion, said Dr. Bandit, it would have been impossible to get the conservative Royal Thai College of Obstetricians and Gynecologists to give up Pap smears, or to persuade Parliament to allow nurses to do cryotherapy, a procedure previously reserved for doctors.
The free screenings at public clinics are crucial to people like Yupin Promasorn, 36, who was part of Miss Maikaew’s group.
She sells snacks in Bangkok, and her husband drives a tuk-tuk motorcycle taxi. With two children, she has no time to wait at Bangkok’s jammed public hospitals, and she is too poor to see a private doctor. So she and her husband drove the 12 hours here, to her native village, in his tuk-tuk. When she found out she was negative, she sat in a chair fanning herself.
“I feel like a heavy mountain is gone from my chest,” she said.